The symptoms of rectal prolapse tend to come on slowly. The first symptom you’ll notice is the feeling that there is a bulge at your anus. It may seem as though you are sitting on a ball.
Normal physical activity, such as walking, sitting, and exercising, may also cause part of the rectum to push through your anus. At first, it can be returned to its proper location by hand.
If rectal prolapse worsens, there could be bleeding from the inner lining of the rectum. In cases of partial or complete prolapse, you may have trouble controlling liquid or solid bowel movement and gas from your rectum.
Up to half of the people with rectal prolapse experience constipation, while others may have episodes of constipation and incontinence.
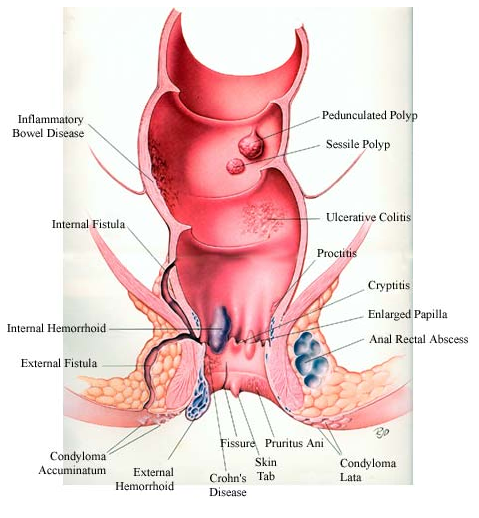
There are three types of rectal prolapse. The type is identified by the movement of the rectum:
- Internal prolapse: The rectum starts to drop, but hasn’t yet pushed through the anus.
- Partial prolapse: Only part of the rectum has moved through the anus.
- Complete prolapse: The entire rectum extends out through the anus.
Rectal prolapse can be caused by several medical conditions. They include:
Nerve damage
If nerves that control the rectal and anal muscles are damaged, rectal prolapse can develop. These nerves can sometimes be damaged from:
- pregnancy or during a difficult vaginal birth
- a spinal injury
- surgery in the pelvic area
- Weakened anal sphincter
This is the muscle that allows stool to pass from your rectum. Common reasons for this muscle to weaken are pregnancy and childbirth, or increased age.
Chronic constipation
The strain of chronic bowel movement problems can make your rectum more likely to move down from its location. Strain while having bowel movements, if done often over a period of years, can also cause rectal prolapse.
While not directly linked to rectal prolapse, some conditions may increase your risk for it, including:
- cystic fibrosis
- diabetes
- chronic obstructive pulmonary disease
- parasitic infections
- a hysterectomy
- Women over the age of 50 are also at an increased risk of rectal prolapse.
Rectal prolapse and hemorrhoids can both be uncomfortable and very painful conditions. Rectal prolapse may initially feel like a bad case of hemorrhoids, and sometimes hemorrhoids on your anus may look as though your rectum is emerging.
Rectal prolapse involves movement of the rectum itself. Hemorrhoids are actually swollen blood vessels in the walls of your rectum or anus. Hemorrhoids, though quite common in their smaller, milder form, can become painful and itchy. They can leave red blood on tissue when you wipe. Rectal prolapse can also cause bleeding sometimes.
Laser Therapy in Piles, Fissure, Fistula
Rectal prolapse won’t get better on its own. The degree of prolapse will increase over time. This process can take months or years, so there isn’t always a rush to make a decision.
If you’ve been diagnosed with rectal prolapse, you may choose to delay treatment if your symptoms are mild enough and your quality of life isn’t significantly hampered.
Surgery is the only way to effectively treat rectal prolapse and relieve symptoms. The surgeon can do the surgery through the abdomen or through the area around the anus.
Surgery through the abdomen is performed to pull the rectum back up and into its proper position. It can be done with a large incision and open surgery, or it can be done laparoscopically, using a few incisions and specially designed smaller surgical tools.
Preventing rectal prolapse isn’t always possible. You can reduce your risk if you maintain good intestinal health. To help avoid constipation, in particular:
- make high-fiber foods part of your regular diet, including fruits, vegetables, bran, and beans
- reduce the amount of processed food in your diet
- drink plenty of water and fluids every day
- exercise most, if not all, days of the week
- manage your stress with meditation or other relaxation techniques
Do’s for All Rectal Cases
- Eat a high-fiber diet (fruits, vegetables, whole grains) to prevent constipation.
- Drink plenty of water (8–10 glasses daily) to keep stools soft.
- Take warm sitz baths regularly to relieve pain and promote healing.
- Maintain proper anal hygiene – wash gently and pat dry.
- Follow the doctor’s prescribed medications and treatment plan.
- Engage in light physical activity like walking to improve bowel movements.
- Use stool softeners or laxatives if recommended by your doctor.
Don’ts for All Rectal Cases
- Avoid straining during bowel movements as it worsens symptoms.
- Do not sit for long hours continuously; take short breaks.
- Avoid spicy, oily, and junk foods that may irritate the rectum.
- Don’t ignore symptoms like bleeding, severe pain, or pus discharge – consult your doctor immediately.
- Avoid lifting heavy weights, which increases abdominal pressure.
- Do not self-medicate or use over-the-counter creams without medical advice.
- Don’t delay surgery or treatment if advised, as conditions can worsen.
